
By Dr. James Augusta
Gastroesophageal reflux disease (or GERD for short) is a common condition affecting overweight and obese patients. It is caused by irritation to the lining of the esophagus by gastric acid or bile. Many people have felt heartburn before, but GERD is a little different.
Symptoms can include:
- Heartburn
- Chest pain
- Difficulty swallowing or food getting “stuck”
- Cough
- Pain felt behind your sternum or breast bone
- Burning of the throat
- Hot, sour or acidic taste in your mouth
These symptoms may be worsened by certain types of food, alcohol, smoking, or even bending over or lying flat particularly after eating a meal. Many factors are involved with severity of GERD including weight, and the presence of a hiatal hernia. A hiatal hernia is located where the esophagus crosses the diaphragm to enter the abdomen. When this opening becomes enlarged it distorts the normal anatomy and can lead to increased reflux symptoms. It can even cause some of the stomach to pull up into the chest.
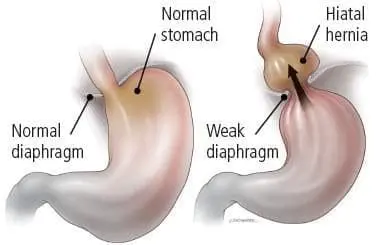
In general, If hiatal hernias are moderate or large we will repair them during your weight loss surgery. If they are small sometimes they are best left alone as making the hiatus too tight can cause issues with swallowing meats and other hard foods.
The two most common options at JourneyLite for weight loss surgery include the gastric sleeve and the Roux-en-Y gastric bypass.
In our experience following a gastric sleeve procedure:
- Roughly 1/3 of patients will develop GERD or their GERD symptoms will worsen.
- Roughly 1/3 get better because:
- weight loss in general can improve GERD or
- the patient had a hiatal hernia that we fixed during the sleeve (see below).
- 1/3 have no change in their symptoms
In contrast, the gastric bypass is actually an increasingly-common surgical treatment for severe GERD. This is because we divert 80-90% of the acid production away from the esophagus with the creation of a small gastric pouch at the top of the stomach. If you do happen to develop severe GERD symptoms after a sleeve gastrectomy (and we are unable to control it with medications), we can convert this to a gastric bypass. In almost all cases this will resolve GERD symptoms, however this would require another surgical procedure and workup (including insurance approval if applicable).
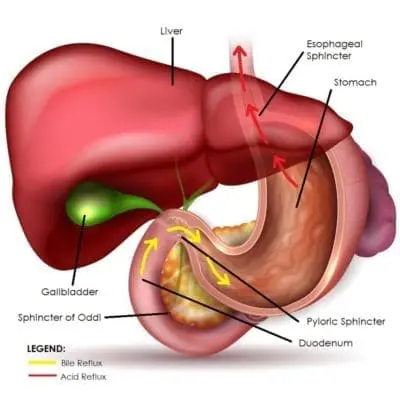
Another condition known as bile reflux can also cause GERD after a gastric sleeve. This is a condition where bile (produced by the liver) comes backwards into the stomach and potentially up the esophagus causing reflux symptoms. Most patients with pre-existing bile reflux will have worsening symptoms after a sleeve. The gastric bypass is also a surgical cure for bile reflux.
For patients with GERD symptoms an EGD (esophagogastroduodenoscopy-an endoscopic camera down the esophagus and stomach) can help you and your surgeon confirm which procedure is best for you. During your consultation, discuss your symptoms and your surgeon can decide if an EGD is warranted. Additionally, if you have already had an EGD done you can request the records be sent to our office for your surgeon to review.
In summary, when considering which procedure is best for you, having a discussion with your surgeon about GERD symptoms is crucial to making the right choice. An EGD can be a good starting point for the surgeon to give recommendations about procedure selection. If you’ve had an EGD done before, you can request the records to be faxed to our office at 513-559-1235. This may save you time and help get your procedure completed sooner. Sometimes it simply comes down to a tradeoff between a gastric bypass with a lower risk of post-op GERD, or gastric sleeve with a higher risk of GERD but a much lower overall long-term risk.

